It is normal to have light bleeding in labor as your cervix dilates and breaks its tiny blood vessels. And as baby emerges from the birth canal there can some local tearing that can cause bleeding. Expect to experience the most bleeding at delivery and postpartum. Most of this bleeding is from where the placenta was located in your uterus.
At normal vaginal birth and immediate postpartum, it is common to lose up to a half liter of blood. After cesarean birth, one liter of blood loss is the average. After birth, your uterus needs to contract around the major blood vessels that supplied the placenta to close them off and prevent excessive bleeding.
The first few days, bleeding can be like a heavy period. Then, it tapers to a moderate period, after which it becomes lighter and changes color over several weeks from shades of red, then pink to brown. The body is healing the former placental site, shedding the internal scab there, and extra tissue and blood that was lining your uterus during pregnancy.
Postpartum hemorrhage usually occurs immediately, or up to the first 24 hours post birth, and remains a major cause of maternal death in the US and around the world. It must be taken seriously. Currently, there is substantial evidence in support of what is termed ‘active management of the third stage of labor,’ to reduce the risk of severe excess postpartum bleeding. It includes the use of:
The synthetic hormone oxytocin (referred to as Pitocin in the US) via intravenous or intramuscular injection
Early cord clamping with waiting 1-3 minutes until baby gets at least most of the cord blood
Controlled traction on the cord along with counter pressure on the uterus to effect placenta delivery within the first 5-30 minutes after birth
Uterine massage to make sure it is firmly contracted
Assessments every 15 minutes for the first two hours.
The above process, or a similar version, is done routinely in most hospitals, and can certainly be done in out of hospital birth settings. However, the studies that determined these procedures, were based on hospital births in mostly resource poor but also well developed countries. Like all studies, they have their limitations and flaws, some were even considered to be of poor quality according to the esteemed Cochrane Review. Also these interventions are not without side effects and concerns. The American College of Nurse-Midwives support the use of active management of third stage of labor in low resource settings, according to their position statement, although they do admit its benefits are not as clear in the low risk healthy population, and encourage the provider to have a risk benefit discussion with each pregnant family so they can make an informed decision about it.
Most homebirth and birth center moms and providers are passionate about physiologic birthing, minimal interventions and holistic modalities, do not routinely want an injection of medication, and are more interested in natural alternatives. They trust the incredible wisdom of the normal birthing process, which has worked for thousands of years or we would not have survived as a species. They share a common belief that if it is not broken, don’t fix it, wary of medication and interventions unless absolutely necessary and benefits outweigh risks. They tend to like the alternative, ‘expectant management’ approach, which also entails close observation by the provider, but tends to take longer, allowing for the normal physiologic process to take its course, and for interventions only if needed in select cases.
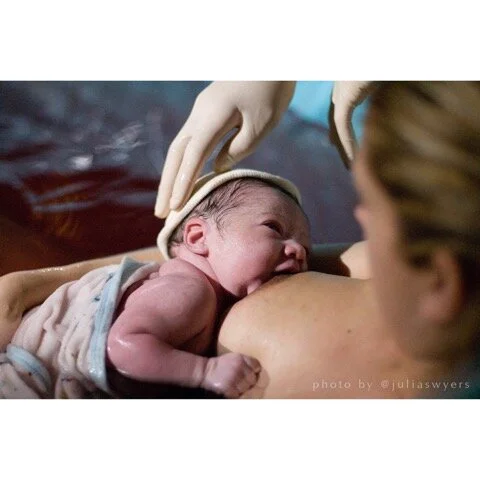
After birth, mom and baby are of course carefully assessed, but encouraged to bond skin to skin. There is no rush. Cord clamping is delayed until pulsation has ceased, or after placenta is birthed. Mom and baby are assisted to breastfeed which helps release mama’s own natural oxytocin.
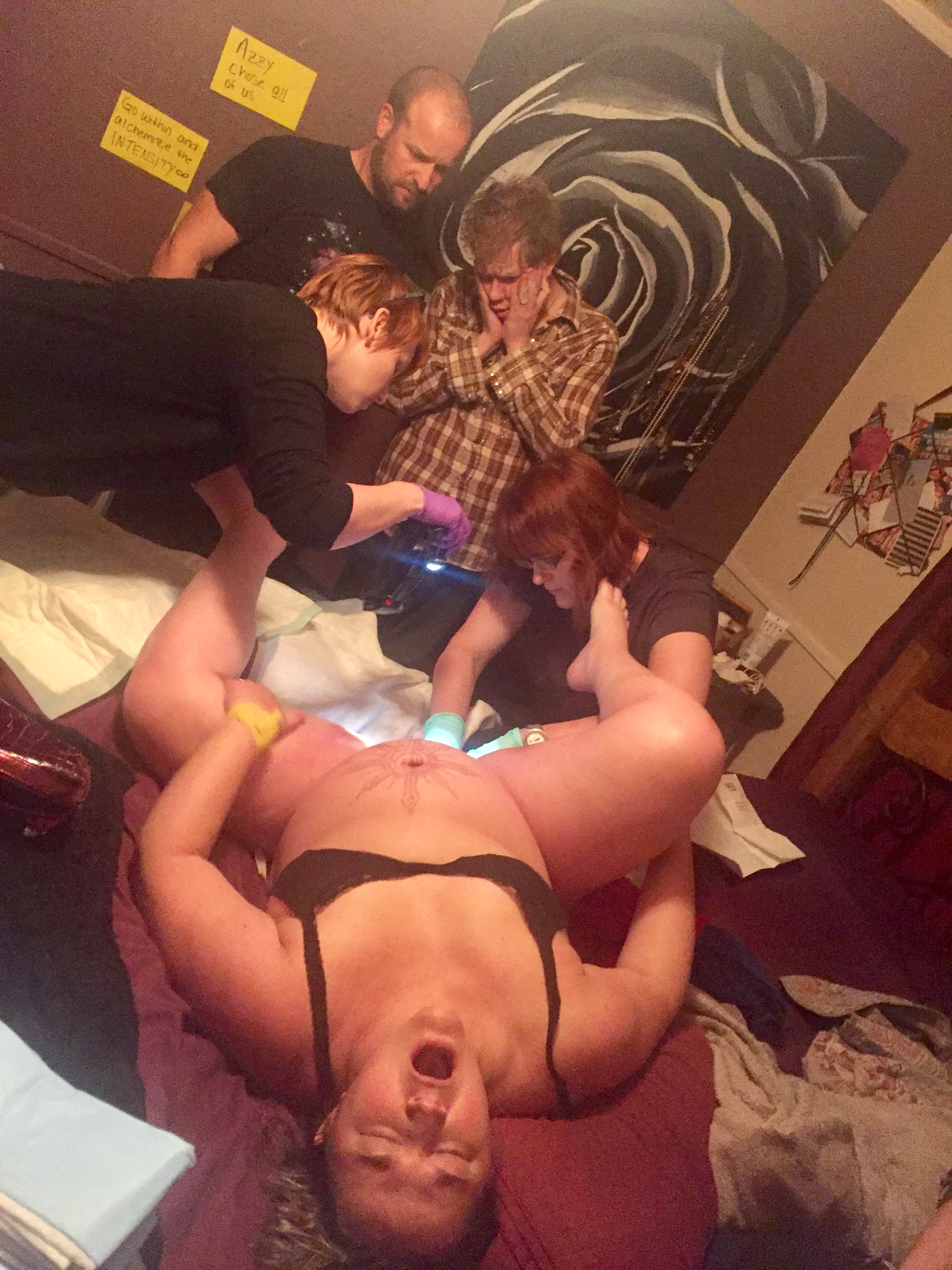
The provider waits and watches for signs that the placenta is naturally separating and then assists mom into an optimal position usually using gravity, and encourages her to use her own bearing down efforts to birth her placenta. The provider may sometimes guide the birthing placenta with gentle traction on the cord, while supporting the uterus, then massages the uterus to make sure it is firm, assesses the bleeding until stable, and assesses and repairs tearing as needed.
Certainly, if there are certain concerns or risk factors, you may truly benefit from medical prevention and active management.
If there is an actual hemorrhage, make sure your provider is skilled, experienced, and fully equipped to deal with it with at least the commonly used effective medications, IV fluids, suturing material for lacerations needing repair, and hands on care that are usually sufficient to control it successfully.
However, you can build up a strong blood supply and reduce excess bleeding and its risks with the following suggestions for natural support both in your pregnancy and postpartum.
Prenatal Support
Make sure you get checked and treated for anemia common in pregnancy, that your iron stores (ferritin) are sufficient.
Eat 3 large servings of wild greens or dark green leafy vegetables every day. They can be made into a salad, lightly sautéed or steamed. Good options are parsley, dandelion, alfalfa, kale, collard greens, comfrey and turnip greens. For additional support, you can try the following:
NETTLE AND RASPBERRY TEA
Starting in the third trimester, drink 1 cup of this nourishing herbal infusion several times per day.
Combine a handful each of the dried herbs Nettles and Red raspberry leaf with 1 quart boiling water.
Steep for at least 4 hours.
Strain to a glass mason canning jar.
You can add fresh mint leaves, lemon juice, or honey to taste.
GREEN DRINKS
Drink 1 ounce fresh, frozen, or powdered wheatgrass juice 1-2 times daily to enrich and build your blood.
Or, try 1 scoop daily of powdered greens in your smoothie, 1-3 Tbsp bottled chlorophyll, or tablets or powders of spirulina and chlorella.
Postpartum
You need to rest in bed, on the couch or an outdoor lounge chair as much as possible for the first 2 weeks to recover. Make sure you arrange for help in the home during this special time. Limiting activity and increasing rest help the area of open uterine blood vessels where the placenta detached to heal.
Check the top of your uterus regularly for firmness, and massage it if it feels soft, until it hardens. Postpartum bleeding can be minimized when mothers are taught regular postpartum self massage of the uterus so that it stays firm and contracted around the blood vessels that supplied the placenta.
Start breastfeeding right away, and every 1 ½ - 3 hours thereafter, especially taking advantage of the times when your baby is awake and alert and eager to suck. Nursing frequently causes the body to secrete its own natural hormone oxytocin to keep the uterus firm and decrease bleeding.
Urinate frequently to keep the bladder empty so the uterus can contract easier.
You can also take homeopathic caulophyllum 30 or 200 C immediately after delivery, then 3-4 pellets arnica 30C under your tongue every 2-3 hours. Or, try herbal shepherd's purse, 1 dropperful of the tincture three times daily for the first 3-5 days after birth. If you need additional herbal support for heavier or persistent bleeding, you can try a dropperful of Angelica tincture a few times daily.
Most of the supplements and herbal remedies I recommend are available on my customized online holistic apothecary. Find the best supplements that have gone through my thorough screening process there. Look in the category for postpartum bleeding prevention or search them individually. My online dispensary is a convenient way for you to purchase my hand-picked, professional-grade, whole food supplements and other natural health products. Ordering is simple, and the products will be shipped directly to your home or work within a few days.
As always, if you need more personal guidance, schedule a consultation with me.
If bleeding becomes heavier than a heavy period, and you are soaking through two maxi pads an hour for 2 hours, empty your bladder, make sure the top of your uterus is firm and massage it if soft until it becomes hard. If no relief, take 1 tsp shepherd’s purse herbal tincture under your tongue. You can repeat the dose a few times, but if the bleeding becomes heavier, contact your practitioner.
Do read my Natural Birth Secrets book, to prepare yourself for a healthy, joyful and calm pregnancy and childbirth - NOW OUT IN SECOND EDITION!
For further inspiration, empowerment, and optimal health in pregnancy, birthing and postpartum, please make sure to take my online Love Your Birth course, so you can ROCK your journey wherever and however you plan to give birth.